Effect of Transcutaneous Vagal Nerve Stimulation and Deep Breathing on HRV
Kristen Sparrow • October 29, 2022

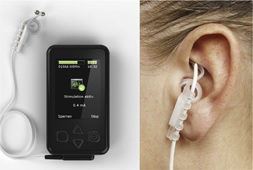 Both deep breathing and TAVNS increased HRV in this study. I discourage patients’ deep breathing while I’m measuring their HRV during acupuncture treatment or acupuncture with TAVNS. The deep breathing distorts the readings wildly. I don’t make a practice of measuring HRV after the intervention has stopped. Maybe I should!!
Both deep breathing and TAVNS increased HRV in this study. I discourage patients’ deep breathing while I’m measuring their HRV during acupuncture treatment or acupuncture with TAVNS. The deep breathing distorts the readings wildly. I don’t make a practice of measuring HRV after the intervention has stopped. Maybe I should!!
Patients with Rheumatoid Arthritis and Lupus have impaired autonomic function, so it makes sense to try to increase their vagal activity.
Jensen MK, Andersen SS, Andersen SS, Liboriussen CH, Kristensen S, Jochumsen M. Modulating Heart Rate Variability through Deep Breathing Exercises and Transcutaneous Auricular Vagus Nerve Stimulation: A Study in Healthy Participants and in Patients with Rheumatoid Arthritis or Systemic Lupus Erythematosus. Sensors (Basel). 2022 Oct 17;22(20):7884. doi: 10.3390/s22207884. PMID: 36298234; PMCID: PMC9607552.
Abstract
Rheumatoid arthritis (RA) and systemic lupus erythematosus (SLE) are associated with an impaired autonomic nervous system and vagus nerve function. Electrical or physiological (deep breathing-DB) vagus nerve stimulation (VNS) could be a potential treatment approach, but no direct comparison has been made. In this study, the effect of transcutaneous auricular VNS (taVNS) and DB on vagal tone was compared in healthy participants and RA or SLE patients. The vagal tone was estimated using time-domain heart-rate variability (HRV) parameters. Forty-two healthy participants and 52 patients performed 30 min of DB and 30 min of taVNS on separate days. HRV was recorded before and immediately after each intervention. For the healthy participants, all HRV parameters increased after DB (SDNN + RMSSD: 21-46%), while one HRV parameter increased after taVNS (SDNN: 16%). For the patients, all HRV parameters increased after both DB (17-31%) and taVNS (18-25%), with no differences between the two types of VNS. DB was associated with the largest elevation of the HRV parameters in healthy participants, while both types of VNS led to elevated HRV parameters in the patients. The findings support a potential use of VNS as a new treatment approach, but the clinical effects need to be investigated in future studies.
Keywords: autoimmune diseases; breathing; deep breathing; heart-rate variability; inflammation; neuromodulation; rheumatoid arthritis; systemic lupus erythematosus; transcutaneous auricular stimulation; vagus nerve stimulation.

