Health & Fitness
Sympathetic Nerves Affect Inflammation More than Vagus N
Kristen Sparrow • December 05, 2019

 According to this study.
According to this study.
I have seen that sympathetic activity does seem to decrease in some patients more than vagal activity increasing with acupuncture and/or TAVNS.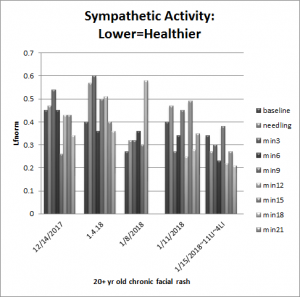
J Physiol. 2014 Apr 1;592(7):1677-86. doi: 10.1113/jphysiol.2013.268573. Epub 2014 Jan 13.
Reflex control of inflammation by sympathetic nerves, not the vagus.
Author information
- 1
- Howard Florey Laboratories, Florey Institute of Neuroscience and Mental Health, University of Melbourne, Parkville 3010, Victoria, Australia. rmca@florey.edu.au.
Abstract
We investigated a neural reflex that controls the strength of inflammatory responses to immune challenge – the inflammatory reflex. In anaesthetized rats challenged with intravenous lipopolysaccharide (LPS, 60 μg kg(-1)), we found strong increases in plasma levels of the key inflammatory mediator tumour necrosis factor α (TNFα) 90 min later. Those levels were unaffected by previous bilateral cervical vagotomy, but were enhanced approximately 5-fold if the greater splanchnic sympathetic nerves had been cut. Sham surgery had no effect, and plasma corticosterone levels were unaffected by nerve sections, so could not explain this result. Electrophysiological recordings demonstrated that efferent neural activity in the splanchnic nerve and its splenic branch was strongly increased by LPS treatment. Splenic nerve activity was dependent on inputs from the splanchnic nerves: vagotomy had no effect on the activity in either nerve. Together, these data demonstrate that immune challenge with this dose of LPS activates a neural reflex that is powerful enough to cause an 80% suppression of the acute systemic inflammatory response. The efferent arm of this reflex is in the splanchnic sympathetic nerves, not the vagi as previously proposed. As with other physiological responses to immune challenge, the afferent pathway is presumptively humoral: the present data show that vagal afferents play no measurable part. Because inflammation sits at the gateway to immune responses, this reflex could play an important role in immune function as well as inflammatory diseases.

